Module 4. Environmental & Exposure Emergencies
How Does Electricity Affect the Body?
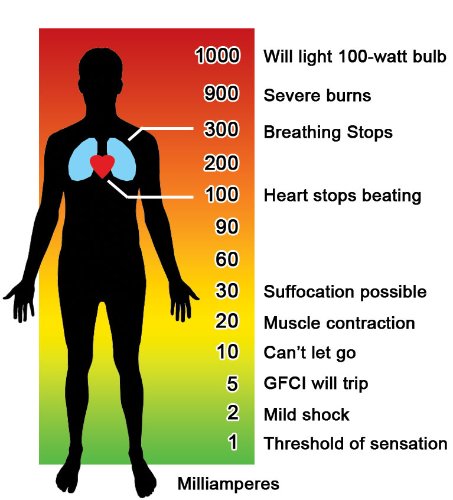
Electricity travels through conductors—materials that allow electrical flow. The human body is an excellent conductor, which is why electric shocks are a common household hazard.
While minor shocks are usually more surprising than dangerous, prolonged exposure or high-voltage electrocution can cause:
- Severe burns to the skin and internal tissues
- Cardiac arrest (disrupting the heart’s electrical signals)
-
Unconsciousness or respiratory failure
×Unconsciousness or respiratory failure
 © FAW Training Solutions – All rights reserved
© FAW Training Solutions – All rights reserved
Important: Electrocution victims may still be in contact with the electrical source. Never touch them until the electricity is turned off.
What to Do in an
Electrocution Emergency
×
Electrocution Emergency
 © FAW Training Solutions – All rights reserved
© FAW Training Solutions – All rights reserved

1. Ensure the Scene Is Safe
- Do not touch the victim if they are still in contact with an electrical source.
- If possible, turn off the electricity at the circuit breaker or power switch.
- If shutting off the power is not possible, use a non-conductive object (plastic, glass, dry wood) to move the electrical source away from the victim.
2. Call 911 If Any of the Following Occur
- The victim is unconscious
- They have burns, difficulty breathing, or irregular heartbeat
- The victim was exposed to high voltage (power lines, industrial accidents)
3. Check for Breathing and Pulse
- If the victim is not breathing or has no pulse, begin CPR immediately.
- If they are breathing but appear weak, pale, or confused, they may be in shock.
4. Treat Burns
- Electrical burns may have both an entry and exit wound (where the current entered and exited the body).
- Cover burns with a dry, sterile dressing. Do not apply ointments or ice.
- Do not pop blisters, as this increases infection risk.
5. Prevent Shock
- Lay the person down with their head slightly lower than their chest.
- Elevate their legs to improve circulation.
- Keep them warm and calm until help arrives.
Note: If they become unresponsive, start CPR immediately.
When to Seek Medical Attention
- The person was exposed to high voltage (power lines, industrial equipment)
- They have burns, chest pain, difficulty breathing, or loss of consciousness
- The victim has tingling, numbness, or muscle weakness after the shock
- They fell from a height or suffered secondary injuries due to electrocution
Even if the person seems fine, electric shocks can cause internal injuries. Always seek medical evaluation after electrocution.
Key Takeaways
- Never touch an electrocuted victim until the power source is confirmed off.
- Use a non-conductive object to separate the victim from the electrical source if needed.
- Call 911 and begin CPR if the victim is unresponsive or not breathing.
- Cover burns with a dry, sterile dressing—do not apply ice or ointments.
- Monitor for signs of shock and seek medical help even if the person appears fine.
Understanding Exposure-Related Emergencies
Extreme temperatures—both cold and hot—can severely affect the body’s ability to function. Without quick intervention, these conditions can cause permanent damage or death.
Hypothermia: When the Body Loses Heat Too Fast
Hypothermia is a dangerous drop in body temperature caused by prolonged exposure to extreme cold. The body fails to generate heat, which can lead to organ failure and death if untreated.
Who Is at Higher Risk?
- People with fatigue, hunger, or poor physical condition
- Elderly individuals and young children
- Those exposed to cold water or prolonged outdoor exposure
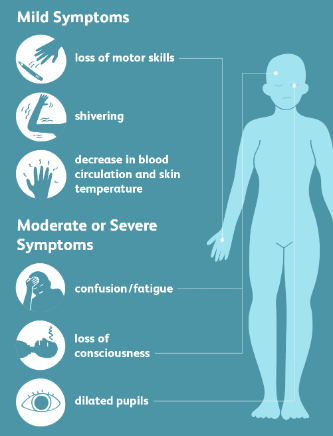
Signs & Symptoms of Hypothermia
×
Signs & Symptoms of Hypothermia
 © FAW Training Solutions – All rights reserved
© FAW Training Solutions – All rights reserved

Mild Symptoms
- Shivering
- Cold, pale skin
- Slurred speech
Severe Symptoms (Life-Threatening)
- Confusion or drowsiness
- Weak pulse and slow breathing
- Loss of coordination
- No shivering (late-stage hypothermia)
- Unconsciousness
First Aid for Hypothermia
- Move the person to a warm, dry place immediately.
- Remove all wet clothing—wet fabrics draw heat away from the body.
- Wrap the person in blankets or use body heat to warm them.
- Give warm (non-alcoholic, non-caffeinated) drinks to increase body temperature.
- Call 911 if symptoms are severe.
Do NOT:
- Use direct heat sources (hot water bottles, heating pads, or fire).
- Give alcohol or caffeine—they increase heat loss by dilating blood vessels.
Frostbite: When Body Tissue Freezes
×
Frostbite: When Body Tissue Freezes
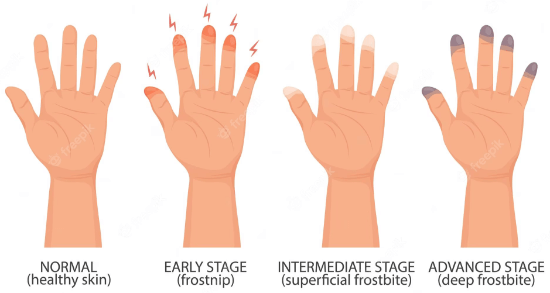 © FAW Training Solutions – All rights reserved
© FAW Training Solutions – All rights reserved

Frostbite occurs when the skin and underlying tissues freeze, typically in fingers, toes, ears, nose, and cheeks.
Signs of Frostbite
- Numbness in affected areas
- White, waxy, or grayish skin
- Hardened, frozen skin
- Blisters (in severe cases)
First Aid for Frostbite
- Apply a loose, sterile dressing to protect the affected area.
- Give warm, sugary fluids (no caffeine).
- Seek medical attention immediately.
Do NOT:
- Rub the frostbitten area—this can cause permanent tissue damage.
- Use heat lamps, stoves, fires, or radiators—these can cause burns.
- Use hot water bottles or boiling water—gradual warming is safest.
Heat Emergencies
Heat Exhaustion vs. Heat Stroke
Heat-related illnesses range from mild to life-threatening. Two of the most common are heat exhaustion and heat stroke. While they may appear similar at first, knowing the difference is crucial—heat stroke is a medical emergency that requires immediate attention.
Heat Exhaustion
- Faintness or dizziness
- Excessive sweating
- Cool, pale, or clammy skin
- Nausea or vomiting
- Rapid, weak pulse
- Muscle cramps
Heat Stroke
- Headache
- No sweating (dry, hot skin)
- Body temperature above 103°F (39.4°C)
- Nausea or vomiting
- Rapid, strong pulse
- Loss of consciousness or confusion
When to Call 911
- The person is unresponsive or confused (heat stroke or severe hypothermia).
- They are not shivering despite cold exposure (late-stage hypothermia).
- Frostbite has turned the skin white, hard, or blistered.
- Cooling efforts for heat stroke are not working.
Key Takeaways
- Hypothermia happens when the body loses heat faster than it can generate it.
- Frostbite is freezing of the skin and underlying tissue, often without the victim realizing it.
- Heat stroke is life-threatening and occurs when the body cannot cool itself by sweating.
- Call 911 for severe temperature-related emergencies.
Understanding Poisoning
A poison is any substance that disrupts normal body functions and can cause serious harm. Poisons can enter the body in four ways:
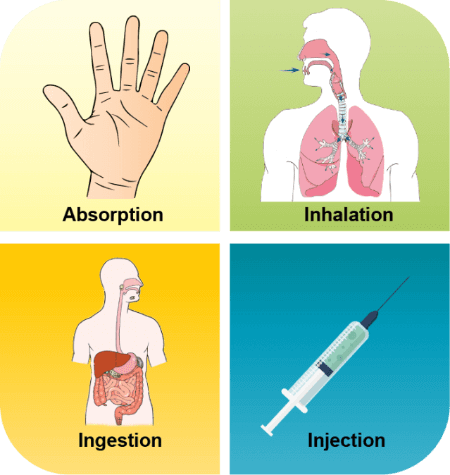
- Ingestion – Eating or drinking harmful substances
- Inhalation – Breathing in toxic fumes or gases
- Injection – Poison entering through a bite, sting, or needle
- Topical Absorption – Poison absorbed through the skin
Poisoning can be life-threatening. Call the Poison Control Center at 1-800-222-1222 or dial 911 in severe cases.
Poisoning by Ingestion
Common Causes
- Overdose of medications, drugs, or alcohol
- Household chemicals (cleaners, detergents, pesticides)
- Spoiled or toxic food
Signs & Symptoms
- Nausea, vomiting, or diarrhea
- Severe stomach pain
- Irregular breathing or pulse
- Burned or stained lips and mouth (from corrosive substances)
First Aid
- Call Poison Control at 1-800-222-1222 for instructions.
- Do not induce vomiting unless instructed by a medical professional.
- In some cases, you may be advised to give water to help dilute the poison.
Do NOT induce vomiting if:
- The substance is a strong acid or alkali (bleach, drain cleaner, battery acid)
- The poison is petroleum-based (gasoline, kerosene, paint thinner)
- The person is unconscious, convulsing, or unable to swallow
If the person is unresponsive or having trouble breathing, call 911 immediately.
Poisoning by Inhalation
Common Causes
- Carbon monoxide from car exhaust, faulty furnaces, or fires
- Industrial chemicals such as ammonia, sulfur dioxide, or hydrogen cyanide
- Smoke inhalation
Signs & Symptoms
- Shortness of breath or difficulty breathing
- Persistent coughing
- Bluish skin (cyanosis) from lack of oxygen
- Bright red skin (in carbon monoxide poisoning)
First Aid
- Ensure the area is safe before entering.
- Move the victim to fresh air immediately.
- Check for breathing and open the airway.
- Start CPR if the person is not breathing.
- Treat for shock if needed.
Call 911 immediately for serious inhalation poisonings.
Note: Carbon monoxide has no smell—install CO detectors in your home.
Poisoning by Topical Absorption
Common Causes
- Chemical burns from acids, alkalis, or industrial chemicals
- Exposure to toxic plants (poison ivy, poison oak, poison sumac)
- Contact with pesticides, fertilizers, or solvents
Signs & Symptoms
- Redness, itching, or burning
- Rash or swelling
- Blisters or peeling skin
First Aid
- Remove any contaminated clothing immediately.
- Wash the affected skin thoroughly with soap and water.
- Apply a topical cream to relieve itching or burning.
- Seek medical attention if symptoms are severe or do not improve.
If the chemical continues to burn the skin, call 911 immediately.
When to Call 911
- The person is unresponsive, unconscious, or struggling to breathe
- Poison Control advises emergency medical attention
- The poison is corrosive, petroleum-based, or taken in overdose
- The person has seizures, chest pain, or signs of shock
Key Takeaways
- Poisoning can occur through ingestion, inhalation, injection, or skin absorption.
- Never induce vomiting unless instructed by Poison Control or a medical professional.
- Always move the person to safety and check breathing and consciousness.
- For skin exposure, remove clothing and wash the area immediately.
- Call 911 or Poison Control for any poisoning emergency.